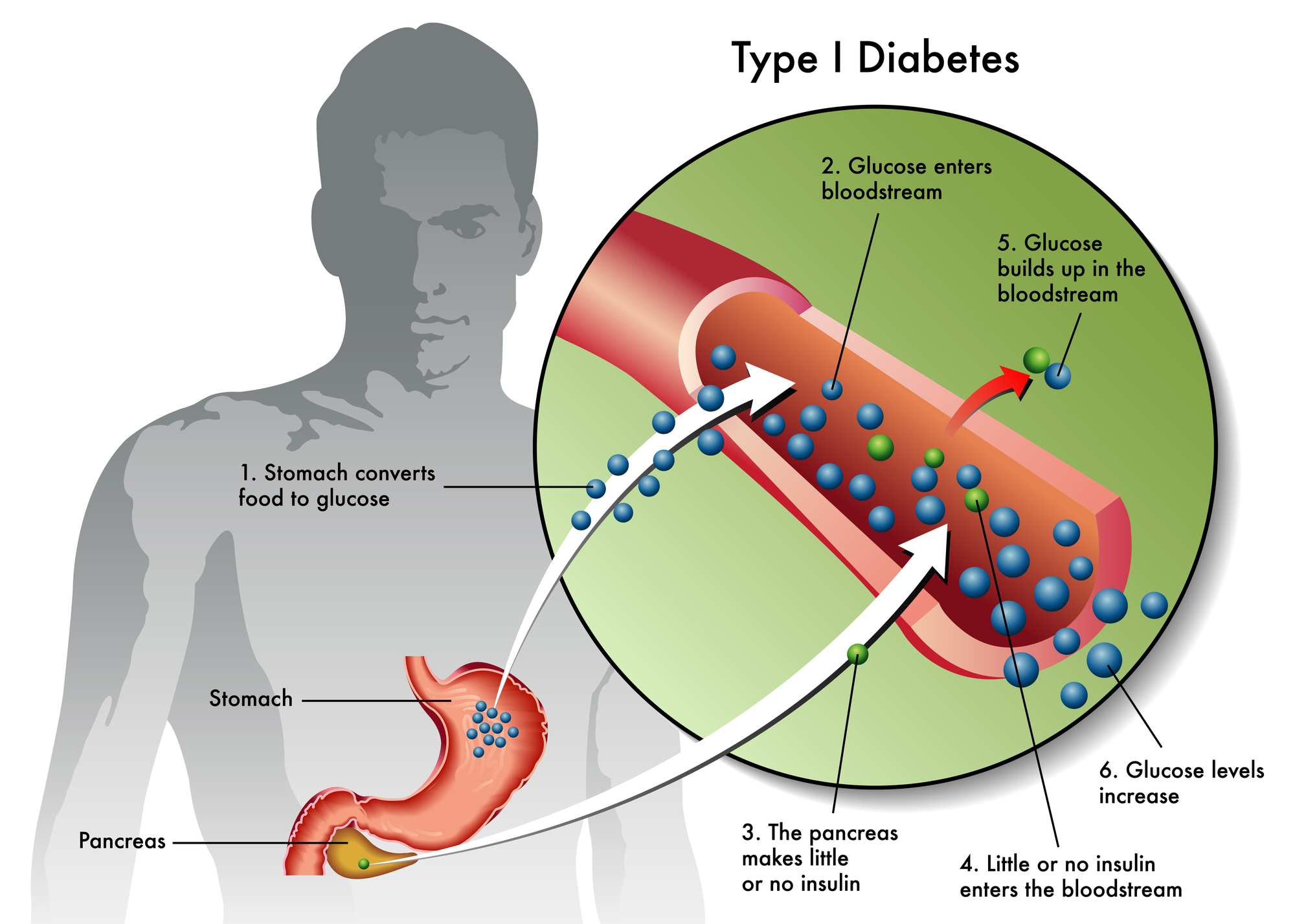
Type 1 diabetes is a chronic autoimmune condition in which the body’s immune system attacks and destroys insulin-producing cells in the pancreas. As a result, people with this condition must rely on insulin therapy to regulate blood sugar levels.
Because of this, researchers have been exploring new approaches within regenerative medicine, including stem cell therapy, to better understand whether pancreatic function could be supported or partially restored.
Here we examine current scientific knowledge, focusing on how stem cells are being studied in relation to type 1 diabetes.
What Is Type 1 Diabetes and How Does It Affect the Pancreas?
Type 1 diabetes occurs when the immune system mistakenly targets beta cells in the pancreas. These cells are responsible for producing insulin, the hormone that helps glucose enter the body’s cells for energy.
As beta cells are destroyed, the pancreas loses its ability to produce insulin. This leads to elevated blood sugar levels, which can cause both short-term and long-term health complications if not carefully managed.
Common aspects of type 1 diabetes include:
- Lifelong dependence on insulin therapy
- Frequent blood glucose monitoring
- Risk of complications such as nerve damage, kidney disease, and vision problems
Because the root cause involves immune system dysfunction and cell loss, researchers are particularly interested in therapies that may address both immune regulation and cellular repair.
For people seeking more detailed information about symptoms, causes, and care options, visiting a resource on treating type I diabetes can provide additional educational insight into how the condition is managed over time.
Stem Cell Therapy: Why It Is Being Studied for Type 1 Diabetes
Stem cells are unique cells that can develop into different types of specialized cells. They also release signaling molecules that may influence inflammation, immune responses, and tissue repair.
One area of research focuses on whether stem cells can help regenerate or replace damaged pancreatic beta cells. Another area explores whether stem cells may help regulate the immune system to prevent further destruction of these cells.
Mesenchymal stem cells (MSCs), commonly derived from bone marrow or adipose tissue, are frequently studied because of their potential immunomodulatory properties. Researchers are investigating whether these cells may help reduce autoimmune activity and create an environment that supports pancreatic function.
These combined effects, immune regulation, and potential cell support make stem cells an important area of interest in type 1 diabetes research.
Can Stem Cells Help Restore Insulin Production?
One of the main questions researchers are exploring is whether stem cells can help restore insulin production in people with type 1 diabetes.
Early-stage studies have examined different strategies, including encouraging stem cells to develop into insulin-producing cells, transplanting stem cell-derived beta-like cells, and using stem cells to support the survival of remaining pancreatic cells.
Some experimental studies have shown that stem cell-derived cells can produce insulin in laboratory settings. In certain clinical research settings, patients have experienced temporary improvements in insulin production or reduced insulin requirements.
However, these results are still being studied. A major challenge is that the immune system may continue to attack newly formed or transplanted cells. Researchers are working to understand how to protect these cells and maintain long-term function.
What Does Current Research Say About Stem Cells and Pancreatic Function?
Current research suggests that stem cells may have several potential roles in supporting pancreatic function, although findings are still preliminary.
Some studies indicate that stem cells may influence immune system activity and reduce inflammation, support the survival of existing beta cells, and promote a more favorable environment for tissue repair.
Clinical trials involving stem cell-based approaches for type 1 diabetes have reported mixed but encouraging results. In some cases, participants showed improved blood sugar control or reduced insulin needs for a period of time.
Researchers are also studying combination approaches that involve both immune therapies and stem cell-based strategies. These approaches aim to address the autoimmune component while also supporting pancreatic cell function.
Despite these developments, experts emphasize that more large-scale, long-term studies are needed to confirm effectiveness and determine how these therapies might be used in the future.
What Do Safety Studies Show About Stem Cell Therapy?
Safety is a critical focus in stem cell therapy. Clinical studies examining stem cell therapies in autoimmune conditions, including type 1 diabetes, have generally reported favorable safety profiles when conducted in controlled environments.
Most reported side effects have been mild and temporary, such as fatigue, low-grade fever, or minor discomfort following procedures. Serious complications have not been commonly observed in many early-stage trials, although ongoing monitoring is essential.
It is important to note that outcomes can vary depending on factors such as the type of stem cells used, how they are prepared, and how they are administered. Because of these variables, continued research is necessary to fully understand both safety and long-term effects.
How Could Stem Cell Research Shape the Future of Type 1 Diabetes Care?
Stem cell research is helping scientists grasp how the immune system and pancreatic cells interact in type 1 diabetes. This knowledge may contribute to future therapies aimed at improving disease management or slowing progression.
Researchers are particularly interested in protecting or preserving remaining beta cells, reducing autoimmune activity, and supporting the regeneration of insulin-producing cells.
While these goals are still under investigation, advances in regenerative medicine may eventually lead to new strategies that complement existing treatments.
For now, insulin therapy remains the cornerstone of type 1 diabetes management, and stem cell-based approaches continue to be studied in clinical research settings.
FAQ About Stem Cell Research and Type 1 Diabetes
- Is stem cell therapy currently approved for type 1 diabetes?
Most stem cell therapies for type 1 diabetes are still experimental and are being studied in clinical trials. - Can stem cells restore pancreatic function?
Some research suggests potential improvements in insulin production, but long-term restoration of pancreatic function has not yet been confirmed. - Could stem cell therapy cure type 1 diabetes?
There is currently no cure. Stem cell therapy is being studied as a possible supportive or future approach, but more research is needed. - Are there risks involved?
Studies generally report mild side effects in controlled settings, though long-term safety continues to be evaluated. - Why is more research necessary?
Large clinical trials are needed to confirm effectiveness, understand long-term outcomes, and determine which patients may benefit most.
Contact Cellebration Wellness on Regenerative Medicine Advances
Scientific research into stem cells continues to expand our understanding of complex conditions like type 1 diabetes. As studies progress, researchers are learning more about how regenerative medicine may influence immune regulation and pancreatic function.
Cellebration Wellness focuses on wellness and regenerative approaches inspired by the latest advances in stem cell research. Educational resources can help you better understand current developments and the science behind emerging therapies.
To learn more about regenerative health education and current developments in stem cell research, contact Cellebration Wellness at (858) 258-5090.