Chronic pain is usually defined as pain that lasts longer than three months or continues beyond normal healing. Unlike short-term pain that fades as the body recovers, chronic pain can persist even when there is no clear injury. It is now understood as a complex condition shaped by interactions between the body, the nervous system, and other underlying processes. According to the National Institute of Neurological Disorders and Stroke (NINDS), chronic pain may continue even after an initial injury has healed and can involve changes in how the nervous system processes pain signals
Because chronic pain does not always respond fully to standard approaches, researchers continue to explore new ways to understand it. One area of growing interest is regenerative medicine, which looks at how the body’s natural repair systems, such as healing responses and inflammation, may be connected to how pain develops and continues over time.
Early research suggests these repair processes may play a role in how pain is felt and maintained. However, results are mixed, and findings can vary depending on the condition being studied. Overall, regenerative medicine remains an evolving area of research, and more studies are needed to better understand its role in chronic pain.
Understanding Chronic Pain
What Is Chronic Pain?
Chronic pain refers to ongoing or recurring discomfort that lasts for months or even years. It may begin after an injury or illness, but in some cases, it continues even after the body has healed. This persistence often reflects changes in how the nervous system processes pain rather than ongoing tissue damage alone.
Chronic pain can affect daily activities, mobility, sleep, and overall quality of life. It may remain constant or fluctuate over time depending on physical, emotional, and environmental factors.
Types of Chronic Pain
Chronic pain is often categorized based on its underlying mechanisms:
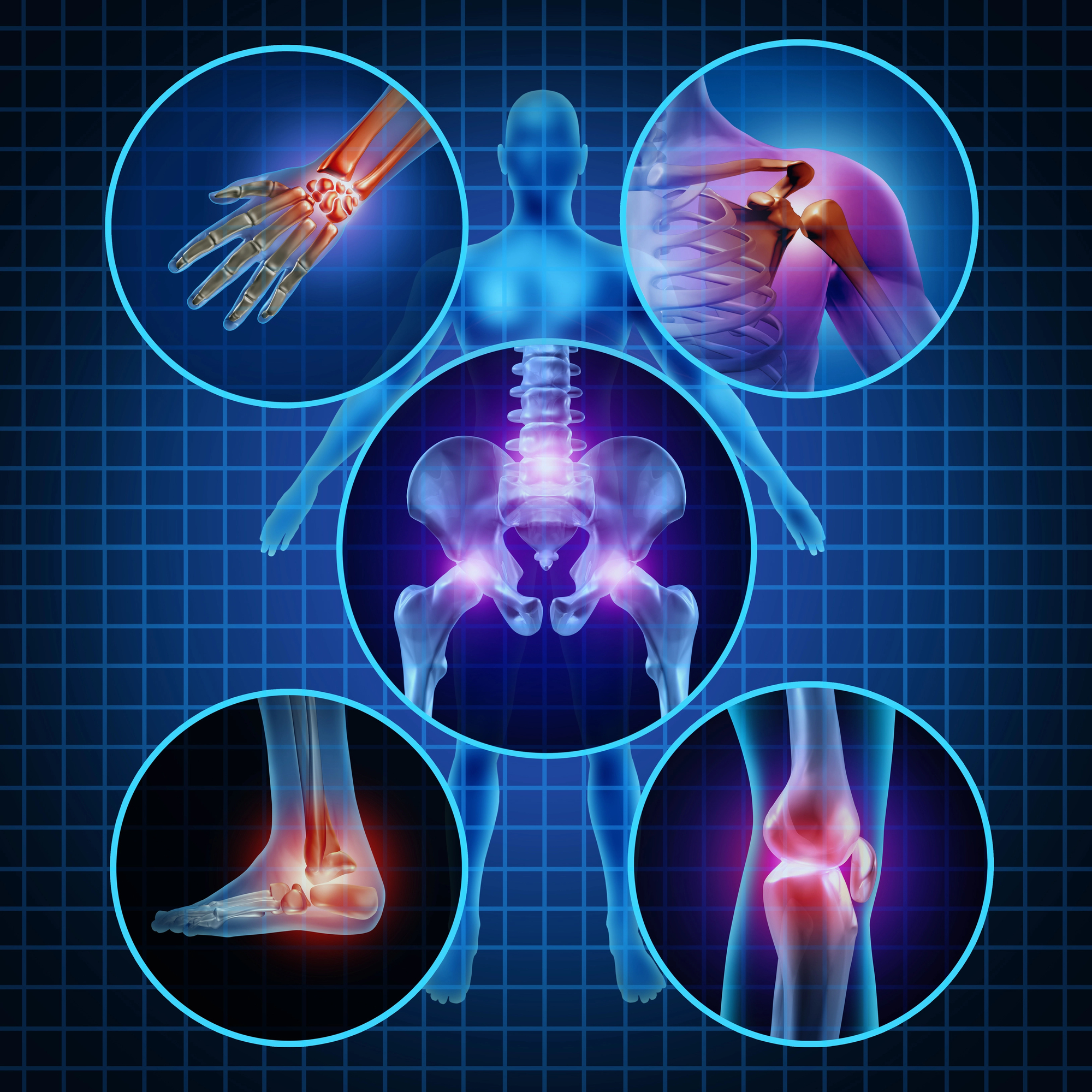
- Nociceptive pain: associated with tissue damage or inflammation, such as joint or muscle pain
- Neuropathic pain: caused by nerve damage or dysfunction, often described as burning or tingling
- Centralized pain: linked to changes in how the brain and spinal cord process pain signals
- Mixed pain: involving a combination of these mechanisms
These categories help explain why chronic pain can feel different from person to person and why treatment responses vary.
Common Causes and Risk Factors
Chronic pain can develop from a range of conditions and contributing factors. Common causes include prior injuries, degenerative conditions like osteoarthritis, nerve damage, and ongoing inflammation. Repetitive strain, physically demanding activities, and poor posture may also increase risk over time.
Additional influences such as stress, sleep disturbances, and overall health can affect how pain is experienced. These factors often interact, making chronic pain a multifaceted condition rather than a single identifiable issue.
The Nervous System and Pain Processing
Pain is processed through a network that includes peripheral nerves, the spinal cord, and the brain. When tissues are injured, signals travel through this system and are interpreted as pain.
Over time, repeated signaling can lead to increased sensitivity within the nervous system. This process, often referred to as sensitization, may cause the body to respond more strongly to stimuli that would not normally be painful. Changes in brain activity and neural pathways may further contribute to how pain is perceived.
Why Chronic Pain Persists
Chronic pain often continues due to a combination of overlapping factors rather than a single cause. These may include:
- Central sensitization, where the nervous system remains highly reactive
- Ongoing low-level inflammation
- Altered communication between tissues and the brain
- Psychological and behavioral influences, such as stress
Together, these elements help explain why chronic pain can persist even when no clear injury is present.
Conventional Approaches to Chronic Pain Management
Common Treatment Strategies
Traditional chronic pain management typically involves a combination of approaches aimed at reducing symptoms and improving function. These may include medications, physical therapy, behavioral therapies, and certain interventional procedures.
Rather than focusing on a single solution, care is often structured as a long-term management plan that adapts over time.
Goals of Traditional Pain Management
The primary goals of conventional approaches are to:
- Reduce pain intensity
- Improve physical function and mobility
- Support long-term quality of life
In many cases, the focus is on helping individuals manage pain effectively rather than eliminating it.
Limitations and Challenges
While conventional strategies can be helpful, they may not address all aspects of chronic pain. Some key challenges include variability in individual response, potential side effects from long-term medication use, and limited impact on underlying biological processes.
These limitations have contributed to increased scientific interest in areas such as regenerative medicine, which aim to better understand the biological drivers of pain.
How Regenerative Medicine Research Approaches Chronic Pain
What Is Regenerative Medicine?
Regenerative medicine is a field of research focused on how the body repairs and restores damaged tissues. It examines cellular behavior, biological signaling, and the tissue environment to better understand healing processes.
Instead of targeting symptoms alone, this research explores how underlying biological systems may influence both tissue health and pain.
Focus on Inflammation and Tissue Environment
Inflammation is a key factor in many chronic pain conditions. While it plays a necessary role in healing, prolonged or dysregulated inflammation may contribute to ongoing discomfort.
Research has explored how inflammatory signals, such as cytokines, affect both tissue function and pain perception. Understanding how these signals are regulated is an important part of studying chronic pain.
Tissue Signaling and Repair Mechanisms
Cells communicate through signaling pathways that guide repair and regeneration. These processes influence how tissues respond to injury and whether healing occurs effectively.
Disruptions in these signaling systems may be associated with prolonged pain. Emerging research examines how modifying the tissue environment could influence these processes and potentially affect pain-related outcomes.
Pain Pathways and Neurological Effects
Chronic pain involves close interaction between physical tissues and the nervous system. Regenerative medicine research explores how biological changes in tissues may influence nerve signaling and pain perception.
Some studies suggest that repair-related processes may interact with pathways involved in pain transmission, including those linked to sensitivity and central processing. However, these relationships are still being studied.
Types of Stem Cells Studied in Research Contexts
Scientific literature commonly discusses several categories of stem cells as part of regenerative research, including:
- Mesenchymal stem cells (MSCs)
- Adult stem cells
- Umbilical stem cells
These cell types are studied for their roles in cellular communication, tissue repair, and biological signaling. Their relevance to chronic pain remains an area of ongoing investigation, and current understanding continues to evolve.
What Current Research Suggests
Overview of Research Findings
Research into regenerative medicine and chronic pain has produced varied results. Some studies suggest that biological repair processes may be associated with changes in pain perception or function. However, these findings are not consistent across all conditions.
Importance of Continued Research
Further research is needed to better understand the relationship between regenerative processes and chronic pain. This includes larger studies, standardized methods, and long-term follow-up to evaluate outcomes over time.
Safety, Limitations, and Regulatory Considerations
Safety Considerations in Research Settings
Safety is a central focus in regenerative medicine research. Potential risks can vary depending on the biological approach being studied and the context in which it is used. Research studies are designed to evaluate both safety and potential outcomes under controlled conditions.
Limitations of Current Knowledge
Current limitations include:
- Limited long-term data
- Variability in research methods
- Incomplete understanding of biological mechanisms
These factors highlight the need for continued investigation and careful interpretation of findings.
Regulatory Landscape
Regenerative medicine research is subject to oversight by regulatory agencies that assess safety and scientific evidence. Some approaches are approved for specific uses, while others remain investigational.
Understanding the distinction between established medical practices and emerging research is important when evaluating this field.
Who Researches Regenerative Approaches for Chronic Pain
Research in this area is conducted by universities, teaching hospitals, and scientific organizations around the world. It involves collaboration between specialists in pain medicine, orthopedics, neuroscience, and biomedical science.
These multidisciplinary efforts contribute to a broader understanding of how biological repair processes may relate to chronic pain and help guide future research directions.
Frequently Asked Questions (FAQs)
- What is chronic pain?
Chronic pain is pain that lasts longer than three months or persists beyond normal healing, often involving changes in the nervous system. - Why is regenerative medicine being studied for chronic pain?
Researchers are exploring how the body’s natural repair systems, including inflammation and cellular signaling, may influence pain mechanisms. - Does research show regenerative medicine works for chronic pain?
Current evidence is mixed. Some studies suggest potential associations, while others show limited or inconsistent results. - Is regenerative medicine safe?
Safety depends on the specific approach and research context. Studies are designed to evaluate potential risks and outcomes. - What conditions are being studied in regenerative pain research?
Common areas include joint conditions, tendon injuries, and certain nerve-related pain disorders. - Is regenerative medicine widely used for chronic pain?
It remains an evolving area of research and is not yet standardized across all aspects of pain management.
Learn More About Chronic Pain and Regenerative Medicine Research with Cellebration Wellness
Exploring chronic pain and regenerative medicine research is an important step when learning about long-term pain and the science behind how it develops and persists. Research in areas like stem cell science and regenerative studies on pain continues to evolve, offering new perspectives on how the body’s natural repair processes may relate to pain alongside conventional approaches.
At Cellebration Wellness, the focus is on education and wellness perspectives inspired by ongoing developments in regenerative medicine research. Speaking with a qualified professional can help you better understand current research, general care options, and what questions to consider when exploring chronic pain management.
To learn more about chronic pain, stem cell research, and regenerative studies on pain, contact Cellebration Wellness today at (858) 258-5090.